Laparoscopy is an operation done under general anaesthetic which allows your doctor to see the pelvic organs (uterus, tubes and ovaries) using a thin telescope called a laparoscope.
Why would I need to have a laparoscopy?
• tubal ligation/sterilisation – where clips are placed on the tubes or removed to prevent further pregnancies
• removal of an ectopic pregnancy (pregnancy outside the womb)
• removal of ovarian cysts
• treatment of endometriosis
• myomectomy (removal of fibroid)
• hysterectomy (removal of uterus)
• treatment of pelvic organ prolapse
What are the advantages of laparoscopy?
Laparoscopy can give a great view inside the abdomen and provides the opportunity to fix many problems through small incisions/cuts. This means you have less pain and a faster recovery. Most operations can be done as ‘day only’ procedures meaning you can go home the same day.
Are there any risks of laparoscopy?
Laparoscopy is a safe operation. However, like with all surgery, it is not completely without risk.
Complications are more likely if you
• Are significantly overweight
• Have had several past abdominal surgeries
Common risks with any surgery
• Problems with anaesthetic
• Bleeding (very rarely needing blood transfusion)
• Clots in the legs (deep vein thrombosis) and lungs (pulmonary embolism)
• Infection of skin cuts, bladder or uterus
Risks of laparoscopy
• A larger cut called a laparotomy is needed to finish the operation or to fix the complications
• Rarely (< 1 %) damage to the internal organs such as bladder, bowel, ureter (tube carrying urine from kidney to bladder) or large blood vessels
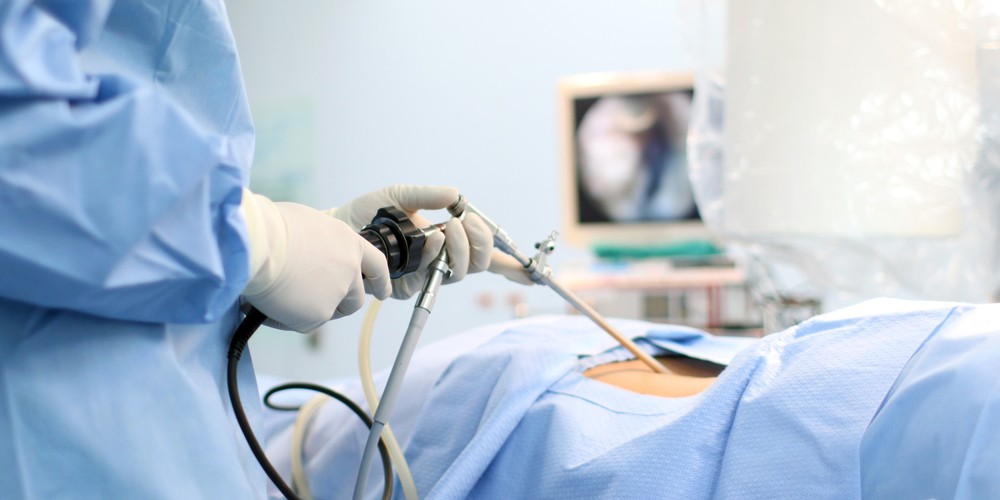
What is involved in a laparoscopy?
Laparoscopy is done under general anaesthetic. A small incision (cut) is made in the umbilicus (belly button) and a thin telescope is placed into the abdomen. Carbon dioxide gas is then fed into the abdomen. Usually 2 or 3 other small 1 cm cuts are made above the pubic hairline or on the sides of the abdomen. These cuts are for instruments which help the surgeons operate. The cuts are usually closed with stitches which dissolve and do not need to be removed. An instrument is usually placed inside the vagina to lift the uterus up so that the pelvic organs (uterus, tubes and ovaries) can be seen clearly.
You will be taken to the recovery ward after the procedure . The nurses will check your vital signs (pulse and blood pressure). They will give you pain relief and medicine to stop any nausea . You will be allowed to go home once you have emptied your bladder, are able to eat and drink, and are feeling well. This is usually 6 hours after the surgery. Rarely patients feel dizzy or unwell and need to stay in hospital a bit longer or even overnight.
Please arrange for someone to drive you home from hospital as you should not drive for 24 hours after an anaesthetic.
What should I expect after the surgery? Tips & tricks for laparoscopic surgery recovery
It is normal to have the following after your laparoscopy for a few days
• mild nausea
• pain around the incisions
• pain in the shoulders or chest wall
• mild period-like pain and light vaginal bleeding
However, you should have a review if you have
• burning and stinging when you pass urine
• heavy bleeding or bad smelling vaginal loss
• increasing abdominal pain
• severe nausea and vomiting or diarrhoea
• fever
• pain, swelling or redness of your legs
• shortness of breath or chest pain
